Listeners:
Top listeners:
00:00
00:00
volume_up
chevron_left
-
 play_arrow
play_arrow
Radio Today Radio Today
-
 play_arrow
play_arrow
Interview: Naudhad Khan on the launch of “Cape Town This Month” Mike Stroud
-
 play_arrow
play_arrow
Interview: Naudhad Khan on the launch of “Cape Town This Month” Mike Stroud
share
close
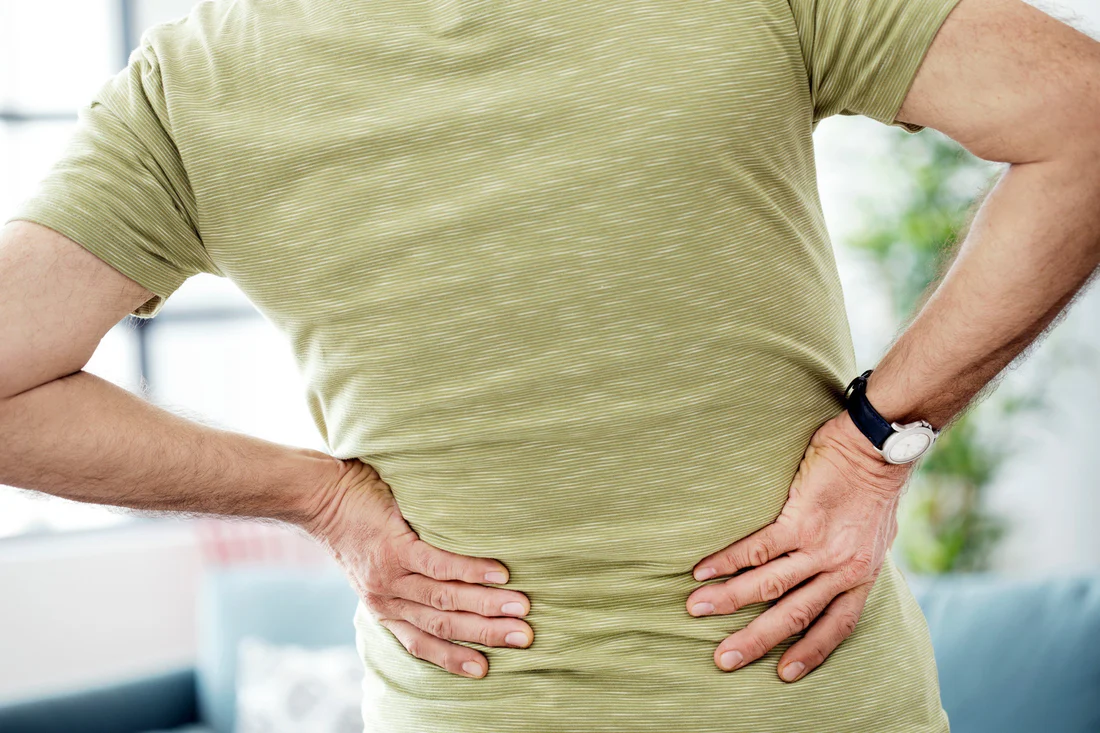
7 Causes of Sacroiliac (SI) Joint Pain (Lower Back Pain)
How to know if you just have a lower-back tweak or if you need to see your doctor.
Key Factors
If you have a dull ache in your lower back that extends down to your buttocks and gets worse when you do things like walk, sit or stand for long periods of time, it could be connected to your sacroiliac joint.
Your sacroiliac, or SI, joints connect your hip bones (ilium) to the triangular bone at the base of your spine (sacrum). Some people have a visible dimple above each butt cheek, along the waistline. That’s where the SI joints are.
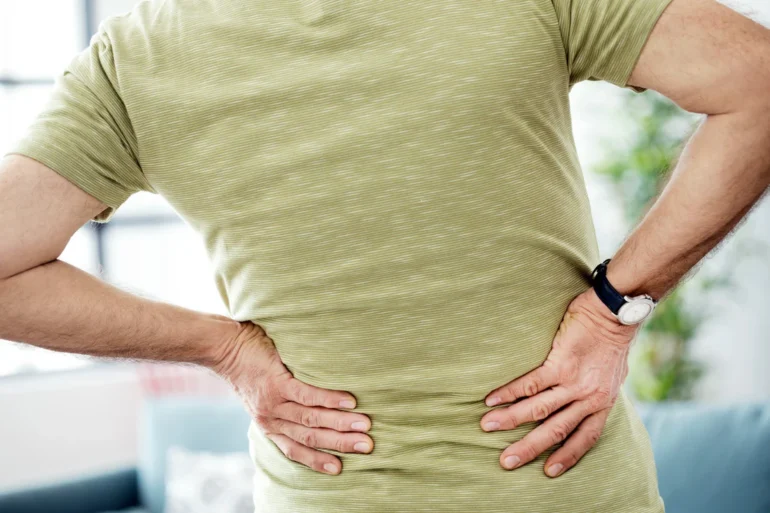
Causes of Sacroiliac pain.
SI joint pain can be caused by several different things, including everything from injury to underlying health conditions. The following are seven common causes of sacroiliac joint pain.
1. Normal wear and tear
“For the 50-and-up population, most SI joint pain is probably just normal wear and tear,” says Dr. Andrew Bach, who specializes in physical medicine and rehabilitation at Cedars Sinai in Los Angeles.
As your body ages, it wears out in some places, including the joints. This could lead to aches and pains in the SI joints, or it could result in full-blown osteoarthritis. This type of arthritis is the most common type, and it’s caused by your bones rubbing against each other and becoming damaged or wearing away over time. If osteoarthritis is the cause of your SI joint pain, your doctor may recommend ways to manage this condition with a combination of medications, exercise, non-surgical procedures and possibly surgery.
2. A fall (or another sudden jolt)
A fall that lands you on your backside can knock your SI joint out of alignment. Other sudden jolts, like stepping off a curb or the bottom step without knowing that step down was there, can wreak havoc on your SI joints as well. A spontaneous lunge to the side — like a move you might make on the tennis court — can throw that joint off kilter, too.“
That’s when you need a physical therapist who’s trained in SI to gently slide it back into place or teach you how to use your own muscles to line it up,” says Valerie Macdonald, a physical therapist at Mass General Brigham Spaulding Rehabilitation in Peabody, Massachusetts. You might also need muscle-strengthening exercises to help hold the joints in place.
3. New repetitive activity (or inactivity)
New repetitive activities that involve the legs, like walking long distances, can cause SI joint pain if you aren’t conditioned for these activities. For instance, if you’re vacationing and doing a lot more walking than you normally do, you might feel the pain in your SI joints.
In these cases, it’s best to avoid whatever activity triggered it. If you walked too much, give yourself a day of rest. If you sat for too long, get moving. An ice pack on your backside right where you feel the pain may help, too.
4. Hypermobility
As the name indicates, a hypermobile SI joint moves more than it should. Specifically, it’s got a little too much wiggle room. The ligaments that connect the sacrum to the ilia (uppermost part of your hip bone) should be tight and range of motion in this joint relatively narrow. But in a hypermobile SI joint, the ligaments are too loose. When the joint wiggles around, it can lead to inflammation and pain.
If this is the cause of your pain, you might manage it with over-the-counter painkillers, physical therapy to strengthen the muscles that hold the joint in place, and supportive devices. Special SI joint belts can be worn under clothing take pressure off the area, resulting in stability.
5. Hypomobility
On the other side of the coin, an SI joint that doesn’t move enough can be painful, too. “When you have a lot of wear and tear, and maybe some arthritis in those joints, you’re probably going to be a little stiffer and a little less mobile,” Bach says.
Aging can also make a difference in how much your SI joints move. “The younger you are, the more mobile that joint is, and when we age, that joint becomes more restricted.” (MacDonald)
As with other symptoms of wear and tear, for SI joint stiffness, your health care provider may offer a combination of pain relievers, exercise recommendations and physical therapy.
6. Ankylosing spondylitis
This type of arthritis is a chronic, inflammatory condition that affects the axial skeleton. “That’s all the midline structures, including your spine, your SI joints, and it can affect your hips, too.
”In advanced cases of this condition, joints, including the SI joints, may fuse, which inhibits motion and causes a great deal of pain. Similar to the treatment for osteoarthritis, treating ankylosing spondylitis typically includes a combination of medications to relieve pain, and exercise and physical therapy to reduce joint stiffness. Severe cases would require surgery.
7. Reactive arthritis
It’s rare, but sometimes an infection somewhere else in the body, such as in the GI tract or the genitourinary system, can lead to inflammation in the joints, including the SI joints. If you’ve recently had a stomach bug, a UTI or an STI, that could be the cause of your SI joint pain. But it usually comes with eye inflammation and pain in the urethra as well. If your doctor diagnoses this as the cause, you may need antibiotics to treat the infection plus medications for your pain.
How is SI pain diagnosed?
It can be difficult for doctors to know for sure that your pain is in your SI joints, since this can be similar to other types of back or lumbar pain. Your doctor might perform a physical exam to rule out other possible causes, and a complete blood test may be done to look for infection or other conditions that could be causing inflammation.
The following may be necessary:
- Pelvis X-rays
- Computed tomography (CT) scan
- Magnetic resonance imaging (MRI)
Treatment of SI Pain
If your pain is mild to moderate, you can try ice and nonsteroidal anti-inflammatories (NSAIDs), like ibuprofen or naproxen. If the pain is from a bout of over or under activity, try doing the opposite for a few days.
Your doctor also might recommend other medications, including:
- Muscle relaxers. These prescription meds may help pain caused by muscle spasms connected to the SI joints.
- Corticosteroids. Steroids can be injected directly into your joint to help with pain and inflammation. But this is usually a short-term solution because repeated injections can damage your cartilage.
- Radiofrequency ablation (RFA). If your pain is bad enough, your provider can permanently block the nerves to your SI joints, though this is not used very often.
You might need to work with a rheumatologist who treats inflammatory diseases if none of these help.
Written by Sonya Collins
Written by: Mike Stroud
Rate it
Similar posts
Recent Comments
No comments to show.Featured post

Latest posts
Current show
Upcoming shows

Breakfast with Errol Ballantine
8:00 am - 10:00 am

Pages Unbound with Glenda Slade
10:00 am - 10:30 am

Living Our Best Years
10:30 am - 12:00 pm

BBC World Midday News
12:00 pm - 1:00 pm

After Lunch with Radio Today
1:00 pm - 3:00 pm
Chart














